
Sign up for a new account.
And get access to
The latest T1D content
Research that matters
Our daily questions
Sign up by entering your info below.
Reset Your Password
Don't worry.
We will email you instructions to reset your
password.
From June 25-29, 2021, the most brilliant minds in diabetes research gathered (virtually) for the American Diabetes Association’s (ADA) 81st Scientific Sessions!
T1D Exchange was honored to present 9 posters and an oral presentation at this year’s conference, covering topics ranging from CGM use and A1c, to the emotional impact of hypoglycemia. Check out the research the T1D Exchange team presented and learn more about each of our studies at the links below!
50-OR: Validation of Fear of Hypoglycemia Screener: Results from the T1D Exchange Online Survey
This study examined the reliability and validity of a newly developed fear of hypoglycemia screener for use in clinics for adults with type 1 diabetes (T1D).
Based on preliminary research, a new fear of hypoglycemia screening tool was developed. The final screener consisted of 9 questions and was then sent to study participants recruited from the T1D Exchange Registry.
The fear of hypoglycemia screener consistently showed that it can reliably assess if a person with T1D needs additional support in this area. Further research is planned to assess the use of this screener in diabetes clinics to help identify those in need and start conversations between healthcare providers and people with T1D about this topic.
51-LB: Emotional Impact of Hypoglycemia and Use of Glucagon: Perspectives of People with Type 1 Diabetes
This study provided insight into the emotional impact of severe hypoglycemia, attitudes toward glucagon, and barriers to using glucagon for people with T1D.
Through 7 focus groups, participants expressed a wide range of emotions about severe hypoglycemia including fear, anxiety, stress, frustration, shame, and embarrassment. The groups described overnight hypoglycemia and CGM alarms as important, however some participants also viewed them as sleep disruptors for themselves and their partners.
Participants in these groups noted that prescription cost and insurance deductibles are some of the biggest barriers to glucagon use. Many people in the focus groups were also concerned about how difficult it can be to prepare glucagon in an emergency.
186-LB: T1D Exchange Registry: Current Insights on Participant Outcomes
T1D Exchange Registry participants complete an initial questionnaire when joining, as well as an annual questionnaire to track changes in their T1D management and outcomes over the course of the year. This study focused on the participants who have been in the Registry for at least one full year and have completed their annual questionnaire.
At the time of the initial questionnaire the cohort reported an average A1c of 7.2% and subsequently 6.8 at the one-year questionnaire. However, 15.0% reported experiencing severe hypoglycemia, while 6.7% reported diabetes-related ketoacidosis (DKA) symptoms over the last 12 months.
This group of Registry participants are highly engaged technology users and meet target A1cs, but still report severe hypoglycemia and DKA symptoms, suggesting that there is still potential for improving outcomes, even among this highly engaged subset of the T1D community.
616-P: CGM Use and A1c: A transatlantic comparison of the DPV Initiative and T1D Exchange Quality Improvement Collaborative (QIC) 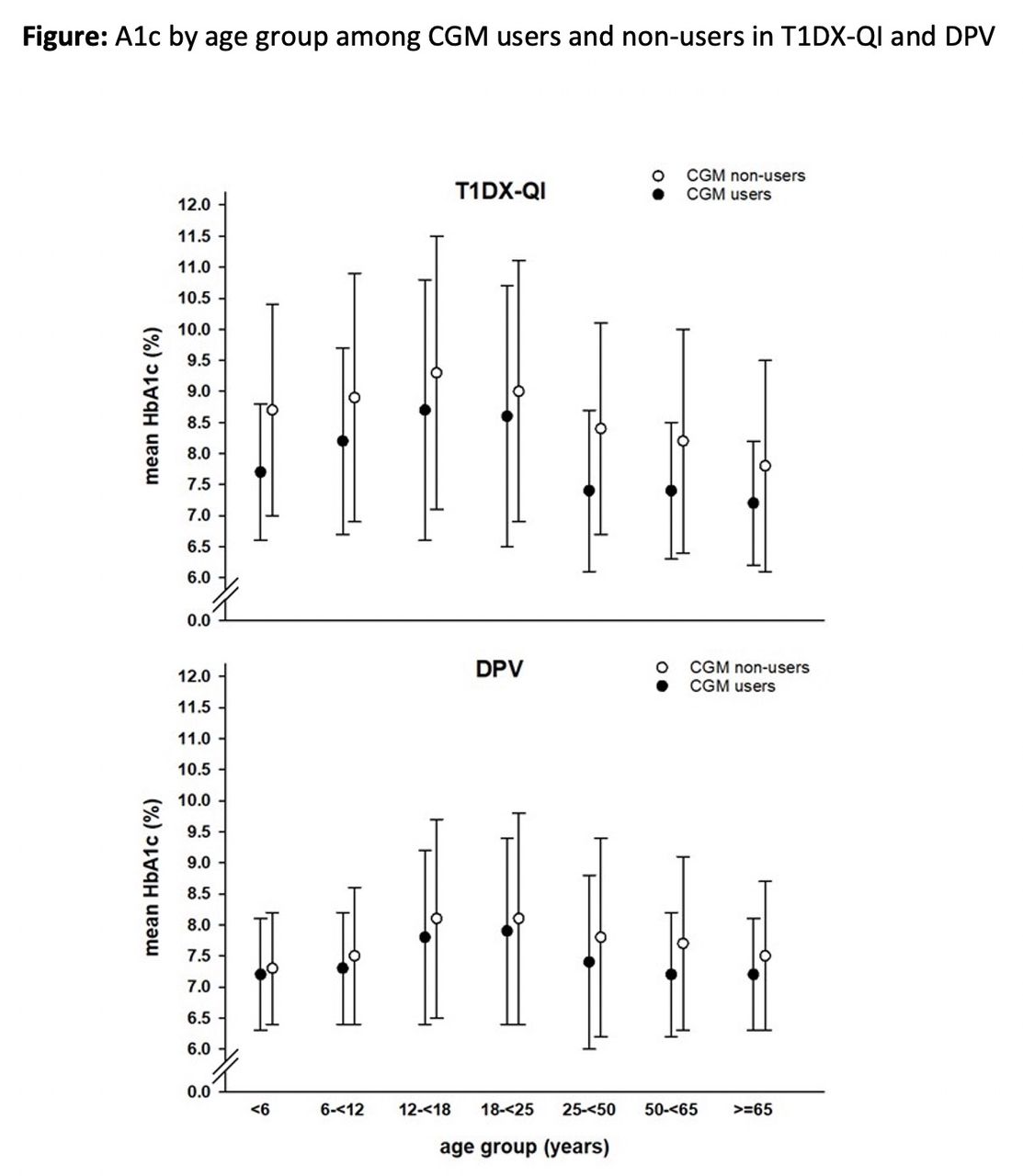
Although it is widely understood that CGMs improve both blood glucose levels and quality of life, the rate of CGM usage varies worldwide. The objectives of this study were to analyze the rates of CGM usage and the association to A1c in the T1D Exchange QIC and the German-Austrian DPV Initiative.
The overall rate of CGM usage in the T1D Exchange QIC was 53.3%, with the highest rate of CGM usage in adults between ages 25 and 49. Comparatively, the rate of CGM usage in the DPV Initiative was 56.3%, with the highest rate of CGM usage in children between ages 6 and 11.
The average A1c was lower in CGM users compared to non-users across all age groups in both the T1D Exchange QIC and DPV, highlighting the need for health policy improvements to promote more widespread usage of CGM worldwide.
822-P: Insulin Pump Use in Patients with Type 1 Diabetes: Real World Data from a Large U.S. Based Multi-Center Observational Study
The goal of this study was to examine the health outcomes in people with T1D who are patients of clinics participating in the T1D Exchange QIC. For this study, we compared outcomes for insulin pump users to non-users.
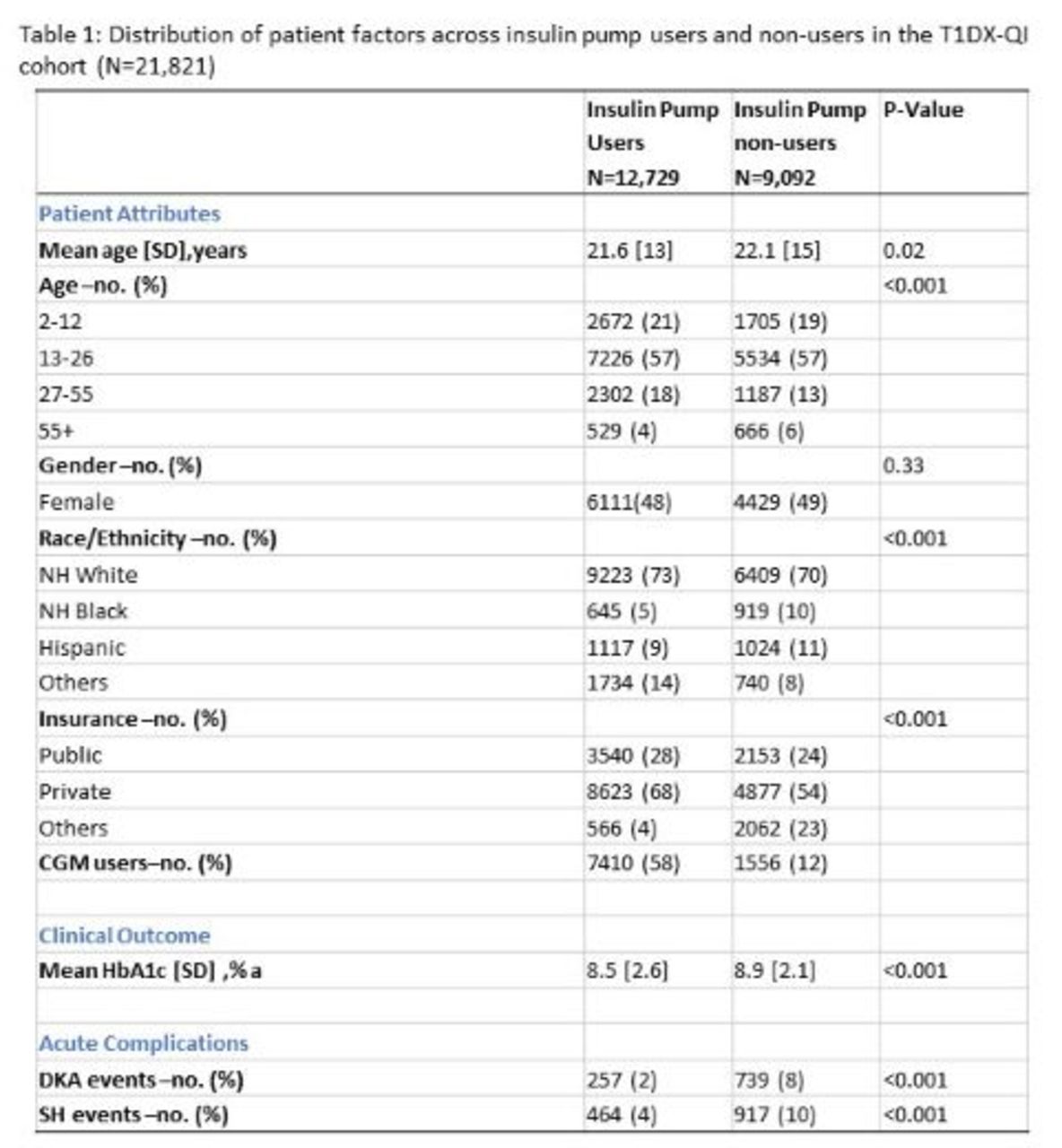
In this group of 21,821 people with T1D, 58% were insulin pump users and 42% were non-users. Average A1c levels among insulin pump user group were 8.5%, compared to non-users, who had an average A1c of 8.9%. Of insulin pump users, 4% reported severe hypoglycemia, compared to 10% of non-insulin pump users. Only 2% of insulin pump users reported DKA, compared to 8% of non-users.
This study confirms previous findings demonstrating the use of an insulin pump to be critical in managing blood glucose levels, especially when used in combination with CGMs.
823-P: Insulin Pump Use and Glycemic Control Among Patients with Type 1 Diabetes: Trends from the Largest U.S. Based Multi-Center Observational Study
For this study, we looked at A1c trends among insulin pump users in eight of the T1D Exchange QIC clinics.
In this group of 15,113 people with T1D, 73% were insulin pump users, and 27% were non-users. The average A1c among insulin pump users was 8.0%, compared to an average A1c in the non-user group of 8.6%. When looking at insulin pump usage across different age groups, this difference in A1c levels was true for people of all ages.
These findings highlight the benefit of insulin pump therapy on achieving target A1c levels for people with T1D of all ages.
833-P: HbA1c trends in the T1D Exchange Quality Improvement Collaborative (QIC) 2017-2020
In 2017, the T1D Exchange QIC began bringing diabetes clinics together to share information, test out new ways of improving care in their clinics and find what works best in the real world.
This study compares trends in A1c levels among patients of these QIC clinics in 2017 when QIC clinics first began working together in this way, versus in 2020 after several positive changes have been demonstrated by these clinics.
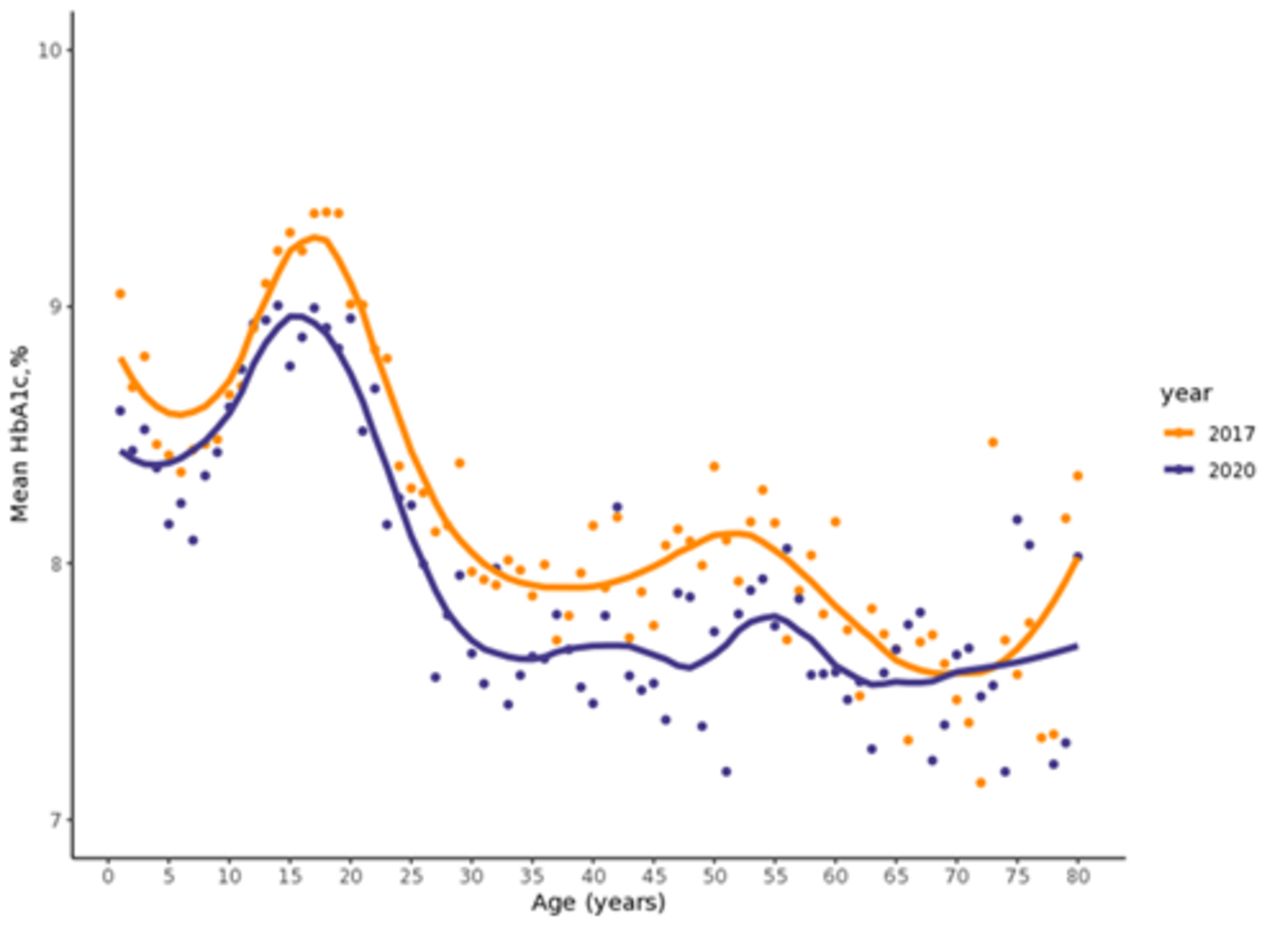 In 2017, the average A1c was 8.9% among people included in this study, compared to the average A1c in 2020, which was 8.6%.
In 2017, the average A1c was 8.9% among people included in this study, compared to the average A1c in 2020, which was 8.6%.
This study demonstrates the early success of the T1D Exchange QIC initiatives. While there are many contributing factors including advances in diabetes technology during this timeframe, this improvement in A1c among QIC clinics is encouraging.
834-P: Factors Associated with Optimal Glycemic Control in Children and Adolescents with Type 1 Diabetes: Real-World U.S. Multicenter Study
Despite advancements in diabetes tech and standards of care, managing blood glucose levels for children and adolescents remains a challenge. This study identified factors associated with an A1c of less than 7% among children in the T1D Exchange QIC clinics.
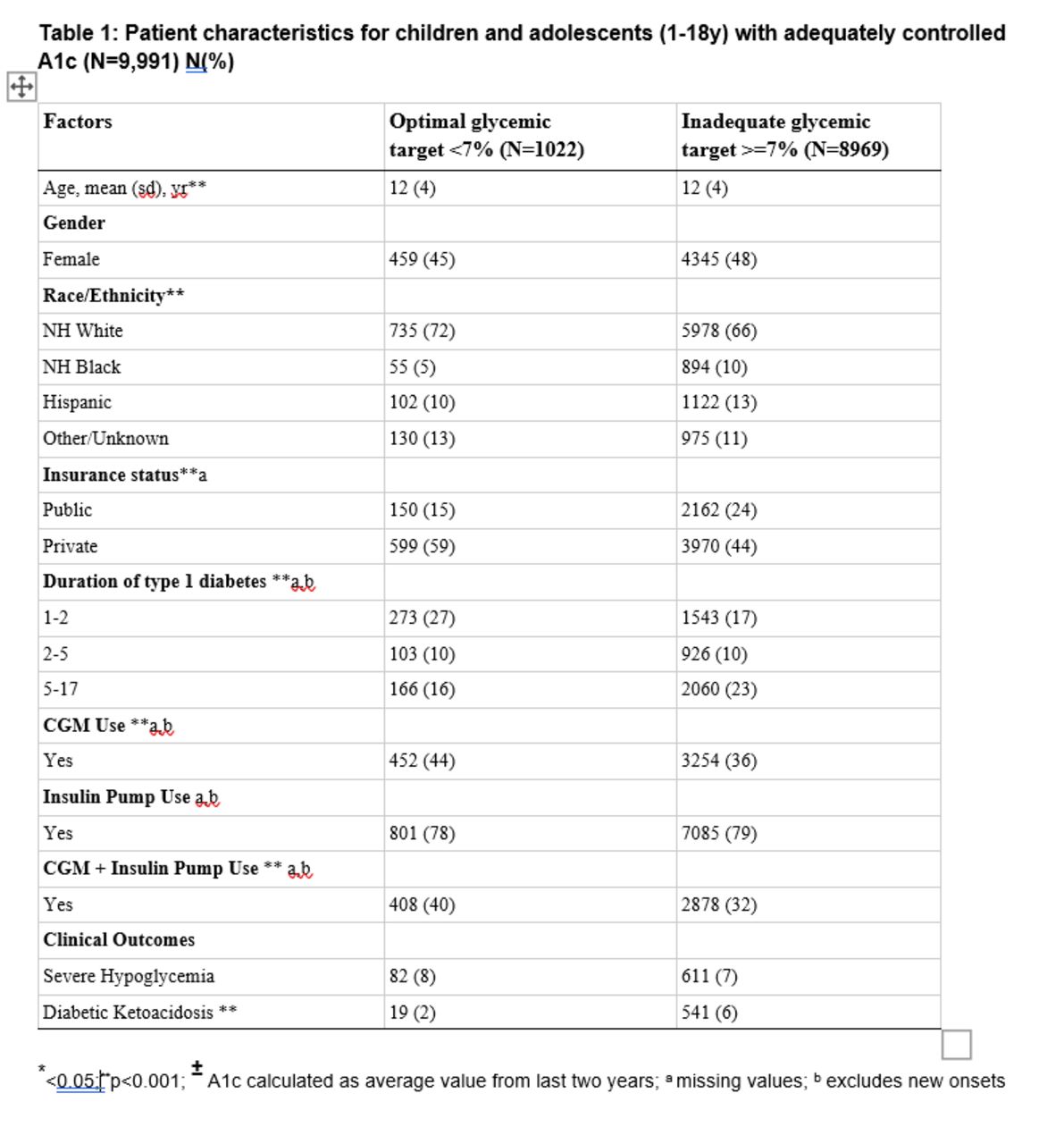 Of the children involved in this study with an A1c below 7%, more were Non-Hispanic White and privately insured compared to people with an A1c greater than 7%. Further analysis showed that children with T1D who used both a continuous glucose monitor (CGM) and an insulin pump were more likely to have a lower A1c compared to those who did not use both tools.
Of the children involved in this study with an A1c below 7%, more were Non-Hispanic White and privately insured compared to people with an A1c greater than 7%. Further analysis showed that children with T1D who used both a continuous glucose monitor (CGM) and an insulin pump were more likely to have a lower A1c compared to those who did not use both tools.
This study highlights the social disparities and real-world challenges of achieving optimal blood glucose management in children with T1D.
850-P: “Six Habits”: Quality Metrics to Support Glycemic Outcomes in Type 1 Diabetes
This study evaluated the relationship of six diabetes self-management habits with A1c.
The “Six Habits” include:
- Checking blood glucose at least 4 times per day or using a CGM
- Administering at least 3 insulin boluses per day
- Using an insulin pump
- Bolusing insulin before meals
- Reviewing data between visits
- Changing insulin doses between visits
Of the 1,212 people with T1D included in this study, A1c was significantly lower for those who performed each habit compared with those who did not. For every additional habit a person performs, we found a 0.7% reduction in HbA1c overall.
861-P: Factors Associated with Optimal Glycemic Management in Adults with Type 1 Diabetes: Results from the T1D Exchange Quality Improvement Collaborative (QIC)
The aim of this study was to identify factors associated with an A1c of less than 7% among adults with T1D in the T1D Exchange QIC clinics.
Among the 8,062 adults with T1D included in this study, 20% had an A1c below 7%. Higher A1c levels were associated with being Non-Hispanic Black, having public insurance, older age, obesity, and high cholesterol.
Improved outcomes were associated with using a CGM, either with or without an insulin pump. On the other hand, optimal blood glucose management was not associated with the use of an insulin pump without a CGM.
These study results highlight the benefits of using a CGM and show the racial disparities and the general difficulty of achieving an A1c below 7% in adults with T1D.







