
Sign up for a new account.
And get access to
The latest T1D content
Research that matters
Our daily questions
Sign up by entering your info below.
Reset Your Password
Don't worry.
We will email you instructions to reset your
password.
Disclaimer: T1D Exchange and the author are not medical professionals. Your target time-in-range may be tailored to your current needs and goals based on discussions with your healthcare providers. Always consult your healthcare team before making any changes to your type 1 diabetes management plan.
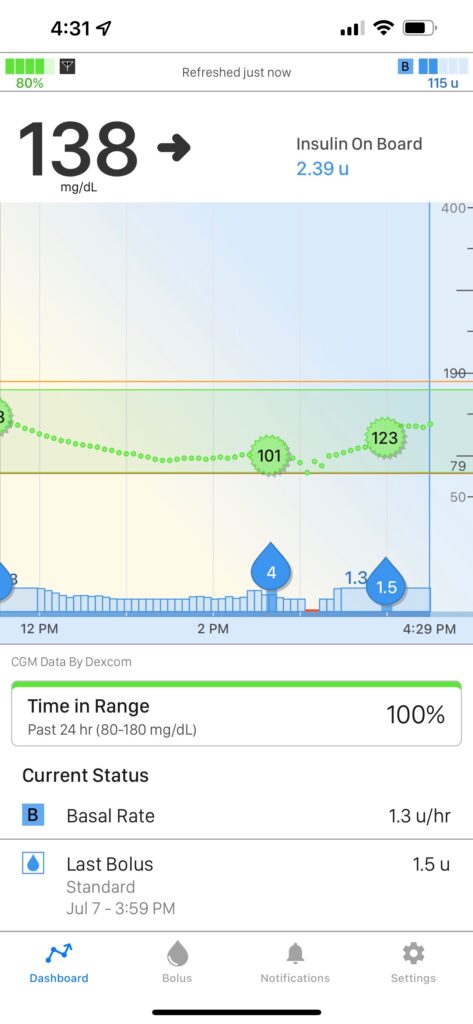
Living with type 1 diabetes (T1D) requires a large toolbox to help manage our blood glucose (BG). Insulin, diet, exercise, a continuous glucose monitor (CGM) and/or blood glucose meter, glycated hemoglobin results (A1C), and more.
But each tool is incomplete on its own. How do we best combine these tools to meet our personal goals? And how do clinical trials measure a tool’s effectiveness to better manage T1D?
Luckily, CGM provides an abundance of data about our BG. From this data, we can calculate our Time in range (TIR), which generally refers to the time spent in a target glucose range. TIR can help those living with diabetes understand if their time spent in hypoglycemia or hyperglycemia is improving over time.
Here we delve into using the powerful tool known as time-in-range.
What’s my time-in-range?
The CDC defines normoglycemia as 70-140 mg/dL. The ADA, ATTD, EASD, and ISPAD each have recommendations, with a goal of at least 70% time spent in the range of 70-180 mg/dL for most people with diabetes. In general, TIR has been categorized as:
| Metric | Definition | Category | Blood glucose (mg/dL) | Goal |
| TAR | Time Above Range | Very High | >250 | <5% |
| High | >180 | <25% | ||
| TIR | Time in Range | Target Range, living with diabetes | 70‐180 | >70% |
| TITR | Time in Tight Range | Normoglycemia | 70‐140 | >50% |
| TBR | Time Below Range | Low | <70 | <4% |
| Very Low | <54 | <1% |
Depending on your situation, however, your recommended target range — or ranges — may vary. For those who are pregnant, a 63-140 mg/dL TIR may be recommended, while 90-150 mg/dL is for those under 18 years old. Consult with your healthcare team to choose ranges that are appropriate for you and your current needs.
TIR and AIC complement each other
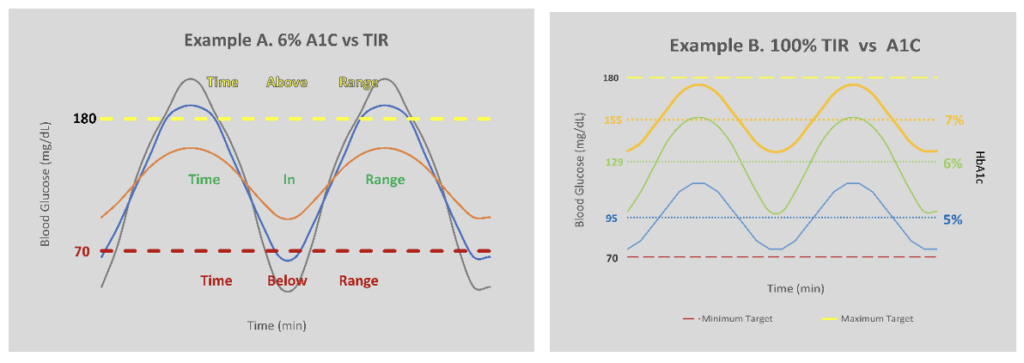
Within a target range, A1C may vary. Example A demonstrates how the same A1C result can have a different TIR, while Example B demonstrates that 100% TIR can have different A1C results.
 The A1C blood test measures the percentage of your red blood cells that have sugar-coated proteins (glycated hemoglobin) and is interpreted as your average BG level over the past 2 to 3 months. But it has limitations: the A1C test is a useful indicator of time spent in hyperglycemia, or TAR, but not hypoglycemia, or TBR.
The A1C blood test measures the percentage of your red blood cells that have sugar-coated proteins (glycated hemoglobin) and is interpreted as your average BG level over the past 2 to 3 months. But it has limitations: the A1C test is a useful indicator of time spent in hyperglycemia, or TAR, but not hypoglycemia, or TBR.
A1C does not reflect the fluctuations of your BG levels throughout the day, nor how factors such as food, exercise, stress, or medication impact your BG. Both hypo- and hyperglycemia can have negative effects on your health and quality of life.
TIR complements A1C to give you a more comprehensive picture of your BG management. Now you can ask yourself:
- What was my TBR at this A1C?
- Why is my A1C higher than expected with my TIR at 70%?
- How can I reduce my TAR after my dinner meal?
Interpreting your TIR
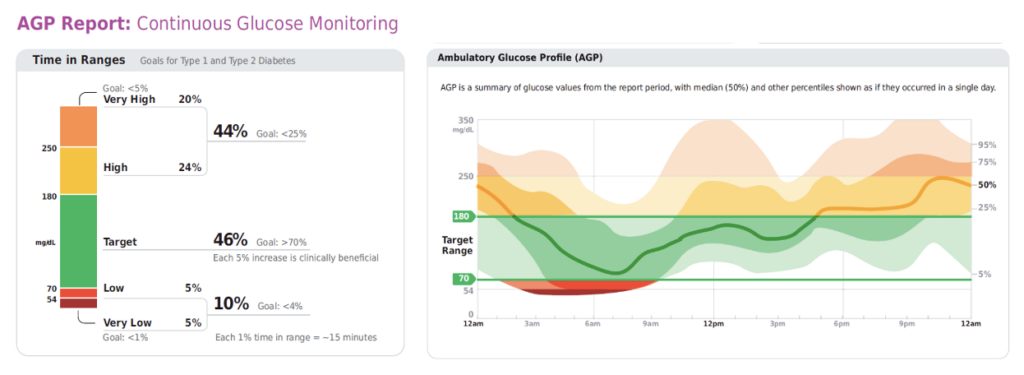
TIR and its subcategories can be calculated from your CGM reports. The Ambulatory Glucose Profile Report (AGP) can help you identify patterns and trends in your BG levels from home, for any date range, with no bloodwork required. Can’t we all use a little less bloodwork?
The AGP examples below are presented in the ADA Standards of Care for Diabetes-2023; your AGP may vary.
 Tips to improve your TIR
Tips to improve your TIR
- Use a CGM device to track your BG levels, get alerts when they are out of range, and make timely adjustments.
- Identify your personal responses to different foods, stress, illness, menstrual cycle, medication, exercise, and more.
- Review your CGM reports regularly to see how much time you spend in, below, and above your target range and identify areas for improvement.
- Consider if automated insulin delivery systems (AID), Looping, new diet and/or exercise regimens, and adjunctive therapies may help meet your TIR goals.
- Work with your diabetes care team to optimize your T1D management plan to achieve your TIR goals.
Reduce your risk of complications
The goal of your TIR is to reduce complications. Studies show that measuring TIR is associated with lower rates of diabetes complications and better outcomes than the A1C result alone.
Improving your TIR can:
- Prevent or delay the onset of diabetic ketoacidosis (DKA), peripheral nerve damage, as well as kidney, eye, and cardiovascular disease from hyperglycemia; Increased TIR was associated with 50–76% reductions in rates of development and progression of microvascular complications.
- Reduce symptoms such as fatigue, headache, confusion, and seizure from hypoglycemia.
Increasing TIR by 10% (or about 2.5 hours per day) is associated with a 64% reduction in the risk of severe hypoglycemia.
TIR and clinical trials
Data from the SURMOUNT-2 trial shows that in those with T2D and obesity, tirzepatide not only promoted weight loss, but it also increased TIR and decreased A1C without severe hypoglycemia. Without the availability and abundance of CGM data, A1C alone could not have reflected the drug’s ability to not increase severe TBR.
Using CGM data, A1C, and the TIR sub-categories, we can hope that clinical studies on new therapies for managing T1D continue to increase!
The FDA and ADA on TIR
The FDA recently issued the draft guidance document on efficacy endpoints: the acceptable metrics demonstrating that an antidiabetic drug is effective in people with diabetes. It is the first update in 15 years to the FDA’s previous recommendations for clinical trials.
While A1C remains the primary endpoint, the FDA now proposes to include CGM-based metrics as supporting endpoints, such as TIR.
If approved, the FDA guidance would align better with the ADA’s recommendation of tailored Standards of Care in Diabetes, such as lower A1C targets when appropriate, and the use of adjunctive therapies that may increase TIR while maintaining or lowering A1C – using caution, of course, to not increase hypoglycemia.
Improving quality of life with T1D through TIR
TIR is a valuable tool that can help you live a healthier and happier life with T1D. By combining TIR with A1C, you can get a more complete picture of your glycemic management to make informed decisions about your personal T1D treatment. Remember that you are not alone on this journey and that you can always reach out to your diabetes care team for support and guidance.
The FDA is accepting comments until August 23, 2023, on its updated draft diabetes efficacy endpoint guidance document. To read the document and submit a comment, visit FDA Docket No. FDA-2023-D-0625.
The ADA is always accepting comments on its Standards of Care living documents at professional.diabetes.org/SOC.
Sources
- Beck RW, Bergenstal RM, Riddlesworth TD, Kollman C, Li Z, Brown AS, Close KL. Validation of Time in Range as an Outcome Measure for Diabetes Clinical Trials. Diabetes Care. 2019 Mar;42(3):400-405. doi: 10.2337/dc18-1444.
- Camerlingo N, Vettoretti M, Sparacino G, Facchinetti A, Mader JK, Choudhary P, Del Favero S; on behalf of the Hypo-RESOLVE Consortium. Design of clinical trials to assess diabetes treatment: Minimum duration of continuous glucose monitoring data to estimate time-in-ranges with the desired precision. Diabetes Obes Metab. 2021 Nov; 23(11):2446-2454. doi: 10.1111/dom.14483.
- de Bock M, Codner E, Craig ME, Huynh T, Maahs DM, Mahmud FH, Marcovecchio L, DiMeglio LA. ISPAD Clinical Practice Consensus Guidelines 2022: Glycemic targets and glucose monitoring for children, adolescents, and young people with diabetes. Pediatr Diabetes. 2022 Dec;23(8):1270-1276. doi: 10.1111/pedi.13455.
- Danne T, Nimri R, Battelino T, Bergenstal RM, Close KL, Devries JH, Garg S, Heinemann L, Hirsch I, Amiel SA et al., 2017, International Consensus on Use of Continuous Glucose Monitoring, Diabetes Care, 40(12):1631–1640, doi: 10.2337/dc17-1600.
- Diabetes Control and Complications Trial Research Group, Nathan DM, Genuth S, Lachin J, Cleary P, Crofford O, Davis M, Rand L, and Siebert C, 1993, The Effect of Intensive Treatment of Diabetes on the Development and Progression of Long-Term Complications in Insulin-Dependent Diabetes Mellitus, N Engl J Med,;329(14):977–86, doi: 10.1056/NEJM199309303291401.
- Diabetes Mellitus: Efficacy Endpoints for Clinical Trials Investigating Antidiabetic Drugs and Biological Products, Guidance for Industry, draft published May 26, 2023. https://www.fda.gov/regulatory-information/search-fda-guidance-documents/diabetes-mellitus-efficacy-endpoints-clinical-trials-investigating-antidiabetic-drugs-and-biological
- ElSayed NA, Aleppo G, Aroda VR, Bannuru RR, Brown FM, Bruemmer D, Collins BS, Hilliard ME, Isaacs D, Johnson EL, Kahan S, Khunti K, Leon J, Lyons SK, Perry ML, Prahalad P, Pratley RE, Seley JJ, Stanton RC, Gabbay RA, on behalf of the American Diabetes Association. 6. Glycemic Targets: Standards of Care in Diabetes-2023. Diabetes Care. 2023 Jan 1;46(Suppl 1):S97-S110. doi: 10.2337/dc23-S006.
- SURMOUNT 2 Trial Results and Potential Role of Tirzepatide in Treating Obesity in Type 2 Diabetes. ADA 83rd Scientific Sessions, Session CT-1.5-SY40. Presented June 23, 2023. New Release accessed June 23, 2023 https://professional.diabetes.org/sites/default/files/media/embargoed_ada_sci_sessions_2023_news_release_surmount_2.pdf
- Blood Glucose Control Studies for Type 1 Diabetes: DCCT & EDIC, National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, website accessed June 27, 2023. https://www.niddk.nih.gov/about-niddk/research-areas/diabetes/blood-glucose-control-studies-type-1-diabetes-dcct-edic
- Centers for Disease Control and Prevention, 2022, National Diabetes Statistics Report website, accessed June 24, 2023. https://www.cdc.gov/diabetes/data/statistics-report/index.html.
- European Association for the Study of Diabetes. Is time in tight range the metric of the future? EASD e-Learning, Horizons News 17th May 2023. https://easd-elearning.org/is-time-in-tight-range-the-metric-of-the-future-news/







