Sign up for a new account.
And get access to
The latest T1D content
Research that matters
Our daily questions
Sign up by entering your info below.
Reset Your Password
Don't worry.
We will email you instructions to reset your
password.
From June 3rd-7th, many of the world’s top scientists in diabetes research gathered in New Orleans for the American Diabetes Association’s (ADA) 82nd Scientific Sessions!
T1D Exchange was honored to have 14 posters and 4 oral presentations at this year’s conference, covering topics ranging from trends in continuous glucose monitor (CGM) and insulin pump use to associations between insurance and A1c.
Check out the T1D Exchange research presented at ADA and learn more about each of our studies at the links below!
92-OR – Persistence of Impaired Awareness of Hypoglycemia, Severe Hypoglycemic Events, and Suboptimal Glycemic Control Despite Advanced Diabetes Technologies
Our partners at Vertex Pharmaceuticals Inc. presented findings from a survey conducted with the T1D Exchange community about how CGMs and hybrid closed-loop systems impact the prevalence of impaired awareness of hypoglycemia, severe hypoglycemic events, and glycemic outcomes.
Although respondents to this survey had high rates of technology adoption, severe hypoglycemic events and hypoglycemia unawareness remained high, with a significant portion of survey respondents not achieving targeted glycemic outcomes.
Read the full article: https://doi.org/10.2337/db22-92-OR
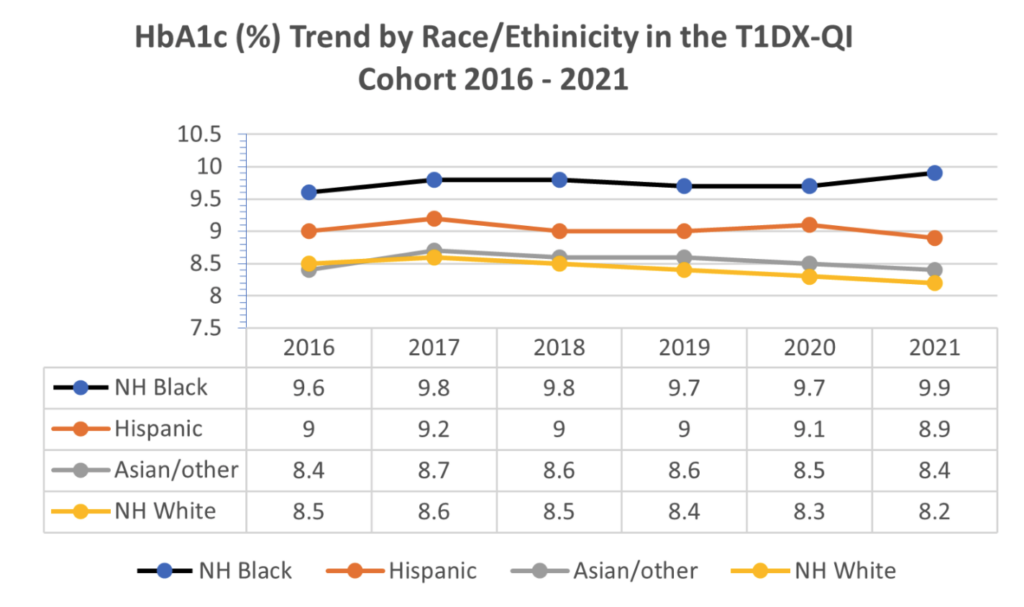
167-OR – Inequities in Glycemic Outcomes for Patients with Type 1 Diabetes: Six-Year (2016–2021) Longitudinal Follow-Up by Race and Ethnicity of 36,390 Patients in the T1Dx-QI Collaborative
Among 36,390 children and adults with T1D, A1c changes from 2016 to 2021 within different racial and ethnic groups were the following:
- Non-Hispanic White: Decrease from 8.5% in 2016 to 8.2% in 2021
- Hispanic: Remained stable from 9.0% in 2016 to 8.9% in 2021
- Asian: Remained stable at 8.4% in both 2016 and 2021
- Non-Hispanic Black: Increased from 9.6% in 2016 to 9.9% in 2021
The use of insulin pumps and CGMs increased significantly among all groups over the six years.
Read the full article: https://doi.org/10.2337/db22-167-OR
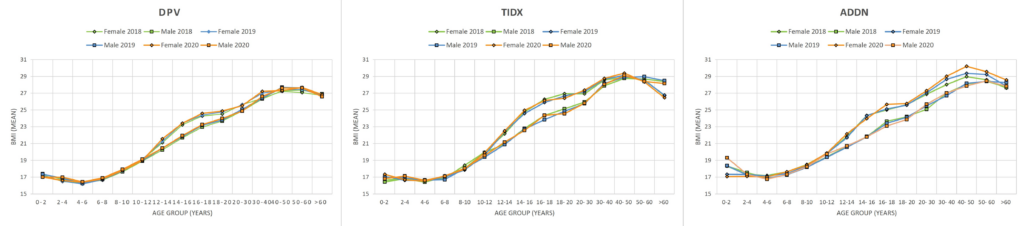
269-OR – No BMI Increase during the COVID-19 Pandemic in Children and Adults with T1D in Three Continents: Joint Analysis of ADDN, T1DX, and DPV Registries
We investigated trends in body mass index (BMI) in three international T1D registries between 2018-2020, including data from the T1D Exchange Quality Improvement Collaborative (T1DX-QI) clinics. To see if restrictions on physical activity and changes in eating habits caused by COVID-19 lockdowns impacted BMI, we looked at average BMIs for March through December of each year.
We found that at a population level, mean BMI was not different before and during the pandemic in people with T1D.
Read the full article: https://doi.org/10.2337/db22-269-OR
289-OR – Automated Insulin Delivery Use among 12,065 T1D Exchange Registry Participants
This oral presentation covers our analysis of T1D Exchange Registry participants to describe the association between automated insulin delivery (AID) usage and A1c, instances of diabetes-related ketoacidosis (DKA) symptoms, and severe hypoglycemia events.
The average A1c was lower in AID users than those using multiple daily injections (MDI) and pumps without AID. Additionally, severe hypoglycemia events were less common among hybrid closed-loop users than those using an insulin pump with predictive low glucose suspend features and MDI users.
Read the full article: https://doi.org/10.2337/db22-289-OR
629-P – Unique Associations between Health Insurance and HbA1c in Adults with Type 1 Diabetes
We examined relationships between A1c and demographics, socioeconomic status, and health insurance type among adults in the T1D Exchange Registry.
Lower A1c was associated with:
- identifying race as White
- higher income
- higher education
- using an insulin pump
- using a CGM
Higher A1c was associated with:
- identifying as female
- having either Medicaid or no health insurance
These results suggest that above and beyond other socioeconomic and demographic factors, health insurance type may contribute to small but meaningful differences in A1c.
Read the full article: https://doi.org/10.2337/db22-629-P
652-P – Gaps Remain in Achieving Target T1D Glycemic Goals Despite Advanced Technologies
This presentation shares some of our work with Vertex Pharmaceuticals, Inc. to analyze CGM data from participants alongside a survey about their experiences with T1D.
Most participants in this study met consensus glycemic targets. However, based on CGM data, participants continued to have significant hypoglycemia, with an average of 1.1 severe hypoglycemia events in the prior year.
Despite improvements in glycemic outcomes such as time in range, time below range, and A1c, many people with T1D still are not achieving clinical targets and are experiencing significant hypoglycemia.
Read the full article: https://doi.org/10.2337/db22-652-P
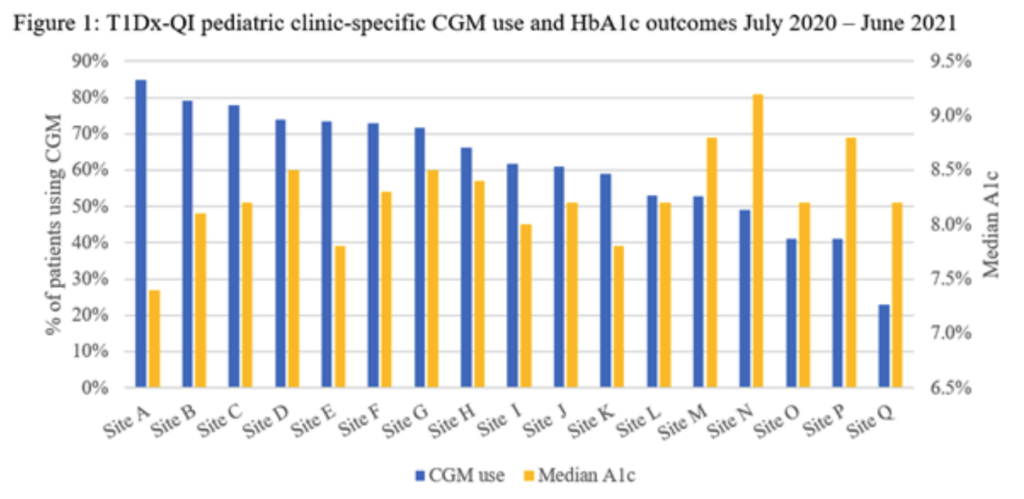
674-P – Benchmarking Continuous Glucose Monitor Use across T1D Exchange Quality Improvement Pediatric Clinics
The T1DX-QI benchmarks key clinical metrics to support quality improvement, share best practices, and promote learning across centers. This study benchmarked CGM usage across 17 pediatric clinics in the T1DX-QI.
The data showed wide variability in the percentage of patients using CGMs across T1DX-QI pediatric centers. Across these 17 clinics, the percentage of patients using CGMs ranged from 23% to 85%, with an average rate of CGM use of about 61.3%
Median A1c values ranged across the 17 clinics ranged from 7.4% to 9.2%, and there was no significant correlation between CGM use and median A1c.
Read the full article: https://doi.org/10.2337/db22-674-P
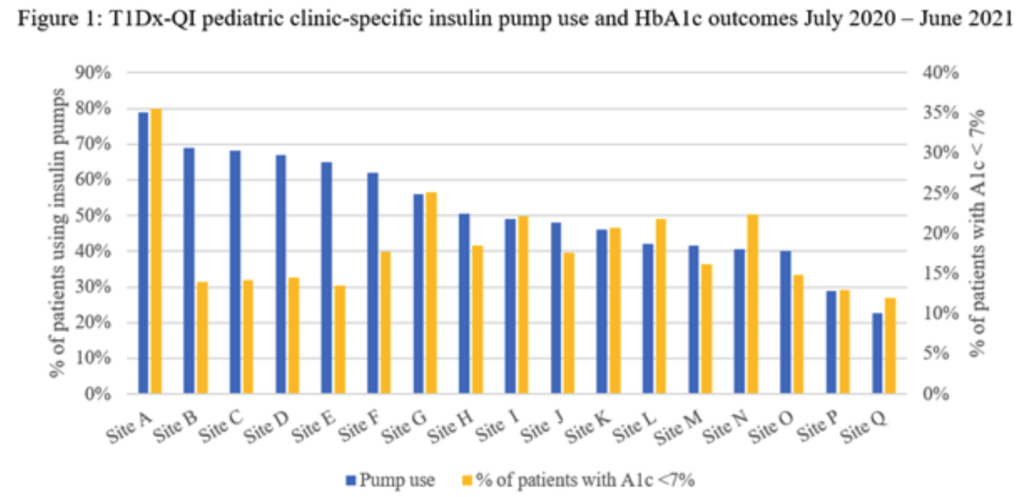
778-P – Variations in Insulin Pump Use across 19 Pediatric Endocrinology Centers in the U.S.
Similar to the above study benchmarking CGM usage in the T1DX-QI, this study benchmarks insulin pump use across pediatric clinics in the T1DX-QI.
Across 17 T1DX-QI clinics, the percentage of patients using pumps ranged from 23% to 79%, with an average of roughly 50%.
Within each clinic, the average percentage of patients with an A1c below 7% ranged from 35% to 12%. There was no significant correlation between pump use and the percentage of patients with an A1c below 7%.
Read the full article: https://doi.org/10.2337/db22-778-P
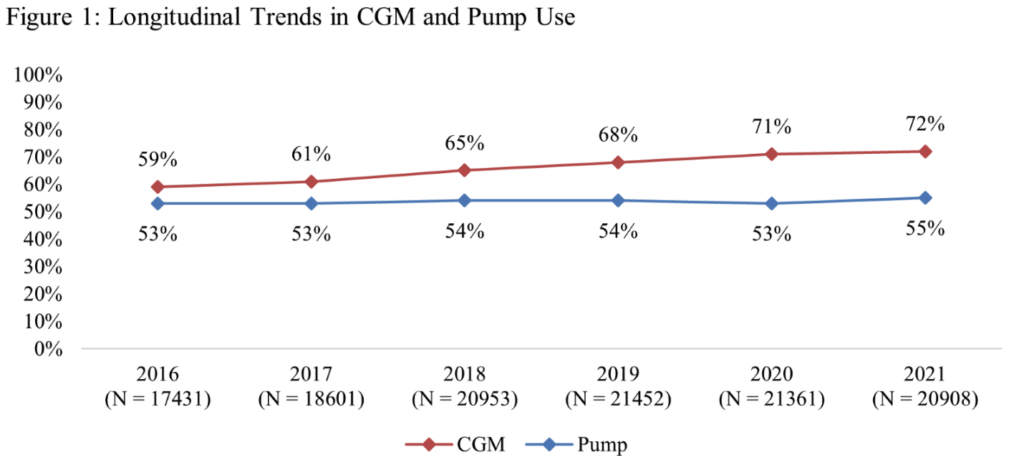
911-P – Longitudinal Trends in CGM and Pump Use: Real-World Data from the T1D Exchange QI Collaborative
This study examines CGM and insulin pump trends between 2016 and 2021, including overall device use and trends by race-ethnicity.
From 2016 to 2021, the percentage of people using CGMs increased from 59% to 72%. Over the same period, the rate of people using pumps remained stable at 54%.
For both devices, racial disparity persisted. There was a 27% and 31% difference in the percentage of non-Hispanic White and non-Hispanic Black people with T1D using CGMs in 2016 and 2021, respectively. There was a 36% and 37% difference in the percentage of non-Hispanic White and non-Hispanic Black patients using a pump in the same years.
Read the full article: https://doi.org/10.2337/db22-911-P
938-P – Implementation of Psychosocial Screening in the Type 1 Diabetes Exchange Quality Improvement (T1DX-QI) Network
This study, which examined psychosocial screening among T1DX-QI clinics, showed varying degrees of screening from clinic to clinic.
Overall, 96% of pediatric centers report using at least one screening tool, and 79% report using more than two tools. 43% of adult centers use one or more screening tools. The most common psychosocial screening in both pediatric and adult clinics is depression.
Centers endorsed multiple benefits of standardized psychosocial screening, including increased provider and patient awareness and the opportunity to discuss psychosocial needs together.
Read the full article: https://doi.org/10.2337/db22-938-P
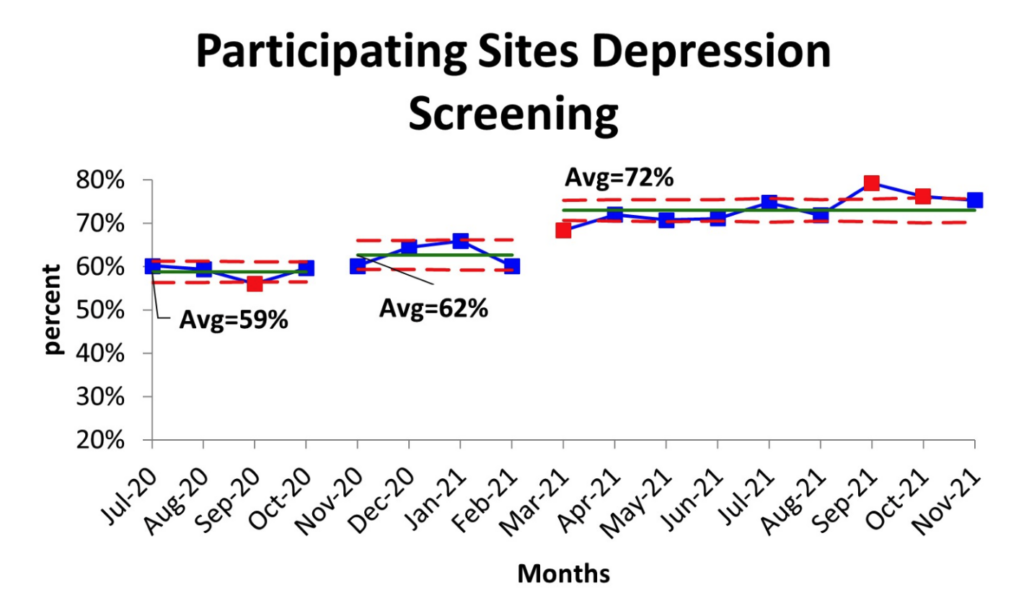
946-P – Multicenter Quality Improvement Project: Increasing Depression Screening across Six Pediatric Endocrinology Centers in the U.S.
Six T1DX-QI centers tried out interventions to expand depression screening in their clinics. Overall, this group of clinics increased their depression screening rate from 59% to 72% over 19 months.
The interventions tested include:
- Use of a screener at visits
- Expanding screening to age 12
- Pulling weekly data to flag patients that should be screened
- Peer support group
- Standardizing screening workflow
- Use of EHR/health information technology
- Provider training
- Monthly meetings to discuss screening protocol
- Streamlining referral process
Read the full article: https://doi.org/10.2337/db22-946-P
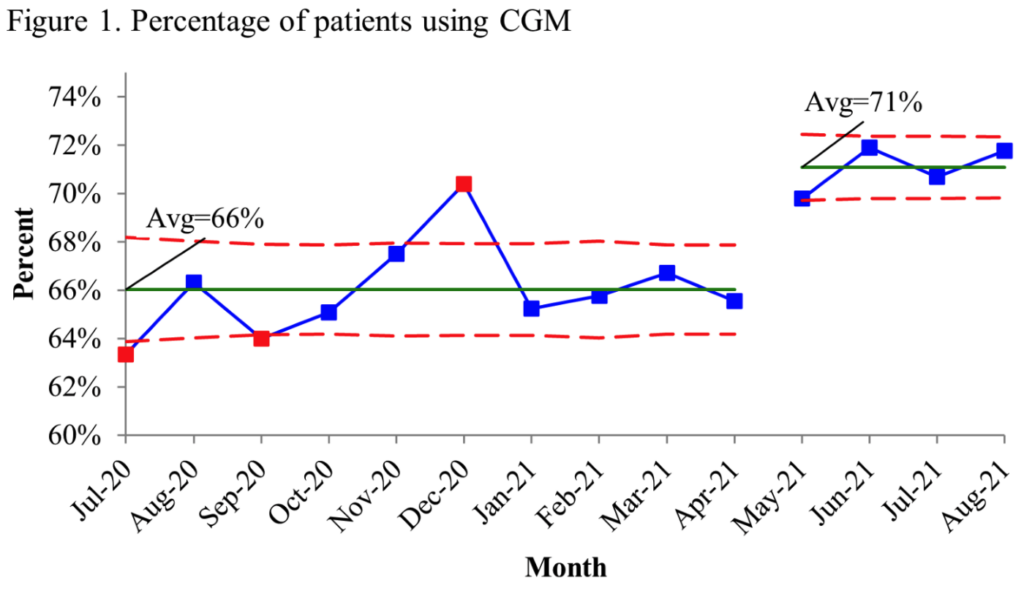
959-P – Improving Continuous Glucose Monitor Use: Success Strategies from the T1D Exchange Collaborative
Seven clinics in the T1DX-QI tested out interventions to expand CGM use. All participating clinics successfully improved CGM use, increasing from 66% to 71% over 14 months. Clinic-level improvement ranged from 5% to 18%, with an average of 9%.
Interventions included:
- Patient education and involvement through print or electronic materials
- Device troubleshooting
- Data downloads
- Optimizing paperwork requirements for new devices
- Standardizing a referral process for patients who face body image challenges
Read the full article: https://doi.org/10.2337/db22-959-P
958-P – Associations between Effect of Body-Mass Index (BMI) and HbA1c among Children and Young Adults with Type 1 Diabetes: A U.S. Based Multicenter Study
The primary objective of this study was to examine the association of overweight and obesity with A1c levels for children and adolescents with T1D.
This study found that A1c levels were higher in the “obese” and “severely obese” groups, with an average A1c of 9.1%, compared to the “normal weight”, which had an average A1c of 8.7%.
Read the full article: https://doi.org/10.2337/db22-958-P
961-P – The Effect of Obesity on HbA1c among Adults with Type 1 Diabetes: A U.S. Based Multicenter Study
Similar to the previous study, we aimed to determine if obesity is associated with increased A1c levels among adults with T1D.
In this study, people in the “obese” group were more likely to have higher A1c levels than people in the “normal” weight group. People within the “obese” group were also less likely to use a CGM or insulin pump.
Read the full article: https://doi.org/10.2337/db22-961-P
971-P – Use of Telemedicine for Type 1 Diabetes Care in the T1D Exchange Quality Improvement Collaborative (T1DX-QI) in 2021
The overall rate of telemedicine among all T1DX-QI centers participating in this study was 37.6% in September 2020 and 20.2% in September 2021, which is a 46% decrease in visits over that year. Telemedicine rates varied widely among centers, ranging from 2.9% to 63.6%.
74.2% of centers in this study had a telemedicine workflow, 35.5% had assigned staff, 71% had support for data uploads, and 51.6% had telemedicine goals.
Read the full article: https://doi.org/10.2337/db22-971-P
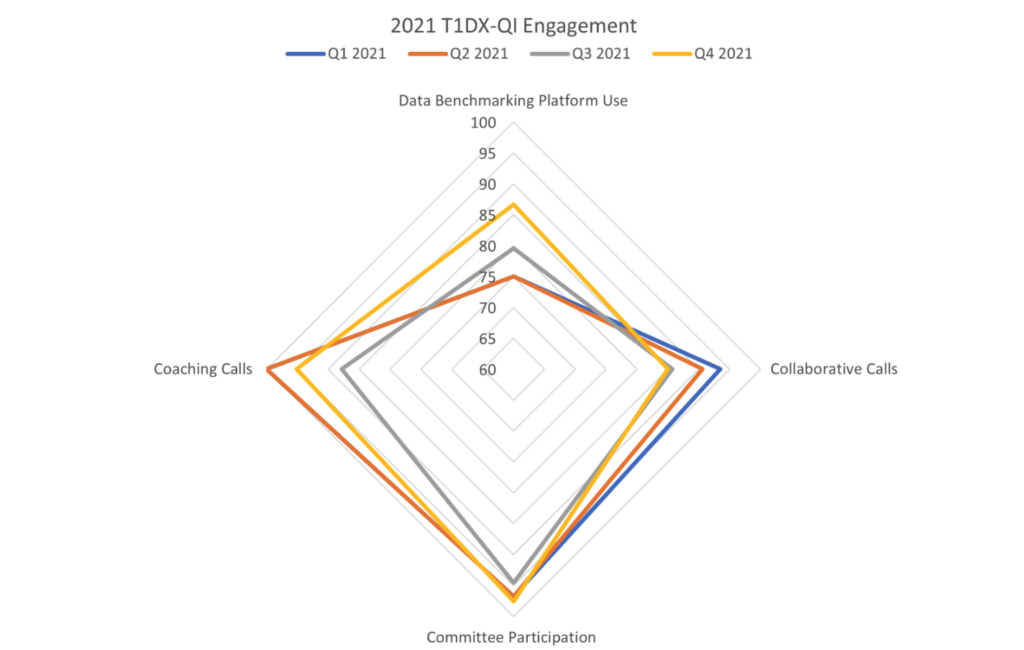
976-P – Measuring Engagement in a National Quality Improvement Collaborative (T1DX-QI)
Clinics that are members of the T1DX-QI have numerous opportunities for engagement, including regular calls that allow for the sharing of best practices and progress made in improvement projects among clinics, one-on-one check-ins with a QI coach, the opportunity to join T1DX-QI committees, and access to an electronic medical record (EMR)-based data platform. Clinics can assess and benchmark their EMR data with other clinics.
From January to December 2021, the T1DX-QI tracked usage of the data benchmarking platform, committee participation, and attendance for collaborative and coaching calls. Over the year, T1DX-QI growth and engagement increased across these measures.
Read the full article: https://doi.org/10.2337/db22-976-P
10-LB – Psychosocial Impact of Severe Hypoglycemia and Perceptions of Nasal Glucagon in Young Adults with Type 1 Diabetes
This study examined whether young adults perceive psychosocial benefits from nasal glucagon.
Of 364 young adults included in this survey:
- Roughly one-third agreed/strongly agreed that possible severe hypoglycemia events limited their engagement in social activities.
- 63.7% agreed/strongly agreed that treating a severe hypoglycemia event was distressing.
- Since having nasal glucagon, 30.9% reported their freedom to engage in social activities improved/greatly improved, and 67.4% reported no change.
Read the full article: https://doi.org/10.2337/db22-10-LB
138-LB – Improving Type 2 Diabetes Medication Prescribing
Two clinics in the T1DX-QI used population health EMR data reports to increase medication prescribing for statins, ACE inhibitors & ARBs, SGLT2 & GLP-1.
Prescribing rates of SGLT2 and GLP-1 increased by 2%, ACE-I and ARB use increased by 1%, and statin rates remained at 73%.
Clinics found that partnering with pharmacists helped to support patients and standardize the process of prescribing medications. Another priority for clinics was planning care so that their teams consistently identified appropriate medications for diabetes and cardiovascular disease management.
Read the full article: https://doi.org/10.2337/db22-138-LB