
Sign up for a new account.
And get access to
The latest T1D content
Research that matters
Our daily questions
Sign up by entering your info below.
Reset Your Password
Don't worry.
We will email you instructions to reset your
password.
Do you store your opened insulin in the fridge? What type of CGM are you currently using? Do you tell the staff at non-diabetes-related appointments that you have T1D? These are this month’s Top Questions of the Day! Your answers inspire research — we’re grateful for your participation!
Here’s a breakdown of August’s most popular Questions of the Day.
(*Comments have been edited slightly for clarity as needed.)
Do you refrigerate your insulin after opening the vial/pen?
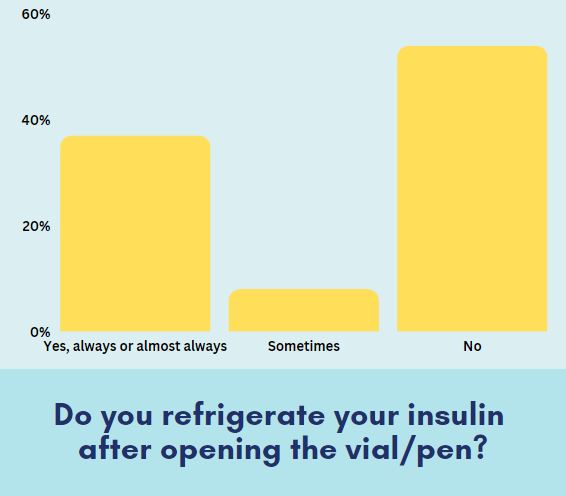
The T1D community loves debating where to store insulin, how long it is safe outside the fridge, and how many days you can get out of a vial! Some people are adamant about storing opened vials in the fridge, while others don’t worry about it. The research on this is a little iffy, too, since insulin’s potency begins to break down about 28 days after being opened.
Here are a few insightful comments from community members:
- “During the summer heat, I use a Frio gel pack using “evaporative cooling,” as it dehydrates. I have used them for years for a pump and then pens. They keep the insulin cool, but not refrigerated.”
- “My answer depends on what type of insulin (I’m MDI): basal insulin from a vial always stays in the fridge, bolus insulin in my pen never does.”
- “I only refrigerate the remaining boxes of my insulin pens, not the ones I am presently using.”
- “Well, they’re different, aren’t they? Pens are meant to be carried around with you, so when I was on MDI, I rarely put the current one back in the fridge. Vials are not, so yes, I always put them back in the fridge after opening.”
- “I have never refrigerated the insulin I am currently using. Been doing this since 1974. Cold insulin leaves bumps of insulin under my skin — no, thank you!”
Do you currently use any of the following CGM systems?
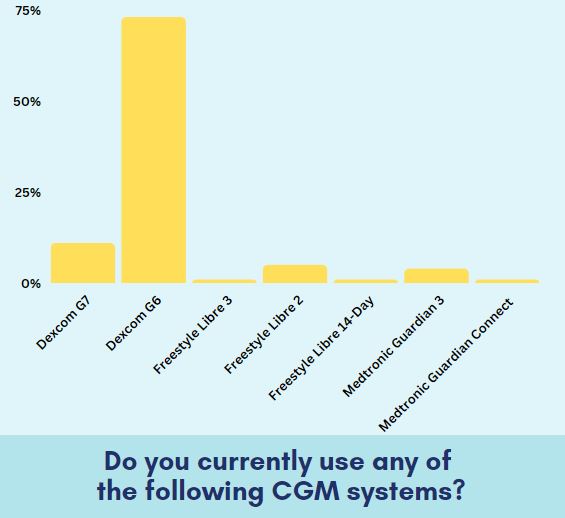
We ask the Online Community this question once every three months because diabetes technology constantly evolves, and preferences change, too. It’s also important to include the latest devices as they become FDA-approved. Many people living with T1D in our community use a CGM to help manage T1D.
Here are a few insightful comments from community members:
- “G6 with Tandem CIQ, and it has been like a CURE! I haven’t Calibrated in over two years, so I don’t need to. In January 2023, my A1C was 5.4. Yep! It has been like a CURE promised almost 60 years ago.”
- “I would switch to the DEXCOM G7, but I am waiting for Tandem to add the software and offer the upgrade. Of course, it will mean updating my prescription and verifying Medicare coverage.”
- “I switched to the G7 when it came out but am now back on the G6. For the G7, the warmup time is only 20 or 25 minutes; the sensor/ transmitter combo is nice and smaller. However, the connectivity to your phone is not very good, and I can’t go into different rooms in my house without it losing the signal.”
- “Finishing up with the Libre2 now that Libre3 sensors are finally available.”
- “Medtronic Guardian 4, amazing auto bolusing.”
If you go to a non-diabetes-related health care appointment, do you tell the staff that you have T1D?
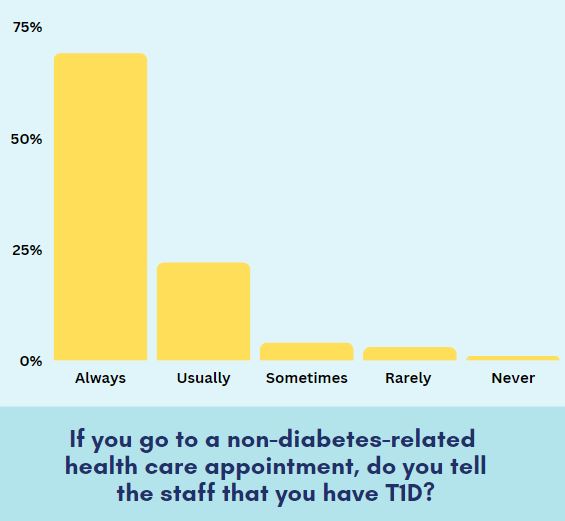
Living with T1D means constantly advocating for yourself, especially at the doctor’s office. Most of our community chose to always tell the staff at non-diabetes-related healthcare appointments that they have T1D, but some members aren’t as vocal. It takes courage and strength to sometimes speak up for yourself, but taking care of yourself should always be a priority. It never hurts to take two seconds to mention to any provider you see that you are living with diabetes.
Here are a few insightful comments from community members:
- “It’s in MyChart, but I often remind them because they see a 47-year-old fat woman and assume type 2. In fact, at a local ER just this summer, I incorrectly “diagnosed” me with type 2.”
- “ALL my doctors know I have T1D. I request all non-diabetic physicians to send a report of my appointment to my endocrinologist.”
- “Only if it comes up in conversation or a recommended treatment is contraindicated due to my T1D.”
- “I hate that I always tell them I have diabetes because some doctors can not pay attention and blame everything on my diabetes.”
- “I think my Type 1 diabetes may affect any other medical issue, including added risks, medicine interactions or effects, healing time, etc. Since diabetes affects the entire human body, I can’t think of a time when it is not pertinent to at least mention it.”
Thank you to every T1D Exchange Online Community member for sharing your experiences. Your words inspire others who come to this community looking for advice and the reminder that they’re not alone.
If you are not a T1D Exchange Online Community member, join today!







