
Sign up for a new account.
And get access to
The latest T1D content
Research that matters
Our daily questions
Sign up by entering your info below.
Reset Your Password
Don't worry.
We will email you instructions to reset your
password.
Editor’s Note: This article was written for awareness purposes only. T1D Exchange and the author do not endorse the use of cannabis, are not medical professionals, and do not give medical advice. T1D patients should always discuss their treatments, disease management, and symptoms with medical professionals.
Many activities impact type 1 diabetes (T1D) self-management: eating, exercising, sleeping, menstruating, working, drinking, healing, and more. Living with T1D means we learn to adjust our insulin and food intake based on the reaction these activities have on our blood glucose levels. Cannabis use is no exception.
Here, we look at recent research identifying a syndrome known as “hyperglycemic ketosis-cannabis hyperemesis syndrome” (HK-CHS) that mimics diabetic ketoacidosis (DKA).
Cannabis & type 1 diabetes today
In the U.S., cannabis remains illegal at the federal level, but is now fully legal in 22 states, and more than half of the states and territories have legalized cannabis for medical use. Use among those living with T1D is also increasing, whether for medical or recreational purposes. Countries like Canada have even gone so far as to issue nationwide best practices to healthcare professionals that treat people with T1D who use cannabis.
Today’s cannabis, in its various forms, has higher concentrations of the active chemical tetrahydrocannabinol, or THC — it is not the cannabis of the ‘60s or ‘70s! And while cannabis is often used to calm nausea and increase appetite, it also dramatically slows gastric emptying. Repeated or extended use can lead to constipation, nausea, acid reflux, and eventually excessive vomiting — or hyperemesis — in any user. Those who live with T1D and use cannabis have 2 to 3 times higher risk of developing DKA.
Additionally, cannabis use can lead to a misdiagnosis of diabetic gastroparesis.
Dr. Halis Akturk and colleagues began noticing patterns among people with T1D in Colorado hospital emergency departments (ED) after cannabis was legalized in the state. They have since conducted several nationwide retrospective studies on those living with T1D that also use cannabis, including hospitalization records and T1D Exchange Registry participant surveys. They found that T1D participants had repeated return visits to the ED in the following weeks, and DKA was frequently misdiagnosed.
Based on that research, Dr. Akturk’s team has recently developed a key to differentiating between DKA and a new syndrome that mimics DKA, one they’ve named HK-CHS: Hyperglycemic Ketosis-Cannabis Hyperemesis Syndrome.
DKA vs. HK-CHS
Many living with T1D are unfortunately familiar with DKA. DKA develops when your body doesn’t have enough insulin to carry blood glucose into your cells to use as energy. Instead, your liver breaks down fat for energy, producing acids called ketones that can build up to dangerous levels in your body — a life-threatening situation. In typical DKA, hyperglycemia (blood glucose >250 mg/dL) precedes ketoacidosis, often accompanied by vomiting, thirst, fatigue, and other symptoms. Left untreated, DKA can be life-threatening.
But when similar symptoms occur in a cannabis-user with T1D, namely vomiting with hyperglycemia, they may be misdiagnosed with DKA. Instead, they may be experiencing HK-CHS, which is characterized by early morning nausea, progressing to severe vomiting that causes ketosis and alkalosis, followed by hyperglycemia.
The key differences for your care team to test are the pH (acid-base profile) and HCO3 (bicarbonate) levels in your blood, along with evidence of ketosis (BHB), as shown below:
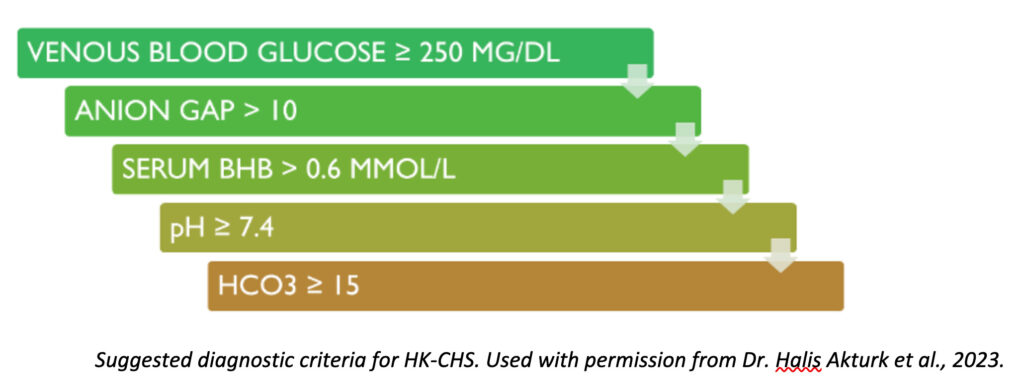
Treating HK-CHS
To treat HK-CHS, your care team will typically increase fluids, treat the high blood glucose with insulin, and balance your electrolytes, or anion gap. You will be advised to stop using cannabis until the symptoms resolve. These treatments will bring your blood glucose levels back into target range and get your gut moving again, which will ease the nausea and vomiting. Depending on your dose, frequency, and duration of use, symptoms may take several days to several weeks to resolve.
If You Use Cannabis and Live with T1D:
- Be honest and forthright with your care team about your cannabis use, just as you would with dietary supplements, alcohol use, or alternative medicines.
- Watch for hyperglycemia and unpredictable blood glucose levels because cannabis slows gastric emptying. Discuss adjusting your T1D management with your doctor.
- Prepare far in advance for tests or surgeries that require fasting, as using cannabis slows gastric emptying. Stopping cannabis use early may help prevent aspirating during a procedure and could prevent a false-positive for diabetic gastroparesis in a Gastric Emptying Scintigraphy test.
- Discuss the impact of cannabis use on your GLP-1 therapy or diagnosed gastroparesis with your care team. Cannabis will worsen your already slowed gastric emptying. Discuss with your doctor what’s right for you in modifying your treatments to avoid complications, including DKA and HK-CHS.
- Tell the ED doctor about your cannabis use, if you present with severe vomiting and hyperglycemia. Remember: an accurate diagnosis of DKA or HK-CHS means you’ll get the proper treatment! Then follow the at-home care instructions carefully.
- Get help if you suspect you have cannabis use disorder, which affects approximately 3 in 10 users. You can contact your healthcare provider, your health department, or your local or regional poison control center at 1-800-222-1222. Dial 911 if it’s an emergency.
Sources
Akturk HK, Snell-Bergeon J, Kinney GL, Champakanath A, Monte A, Shah VN. Differentiating Diabetic Ketoacidosis and Hyperglycemic Ketosis Due to Cannabis Hyperemesis Syndrome in Adults With Type 1 Diabetes. Diabetes Care. 2022;45(2):481-483. doi:10.2337/dc21-1730
Akturk HK, Taylor DD, Camsari UM, Rewers A, Kinney GL, Shah VN. Association Between Cannabis Use and Risk for Diabetic Ketoacidosis in Adults With Type 1 Diabetes. JAMA Intern Med. 2019;179(1):115–118. doi:10.1001/jamainternmed.2018.5142
Bajaj HS, Barnes T, Nagpal S, et al. Diabetes Canada Position Statement on Recreational Cannabis Use in Adults and Adolescents With Type 1 and Type 2 Diabetes. Can J Diabetes. 2019;43(6):372-376. doi:10.1016/j.jcjd.2019.05.010
Camsari, Ulas M. MD1; Akturk, Halis K. MD2; Taylor, Daniel D. DVM, MPH3; Kahramangil, Doga MS2; Shah, Viral N. MD2. Unhealthy Cannabis Use among Recreational and Medical Cannabis Users with Type 1 Diabetes. The Canadian Journal of Addiction 10(3):p 38-41, September 2019. | DOI: 10.1097/CXA.0000000000000061
Center for Disease Control and Prevention. Marijuana and Public Health Publications, accessed 8 February 2023 at https://www.cdc.gov/marijuana/featured-topics/what-we-know-about-marijuana.html
Kinney GL, Akturk HK, Taylor DD, Foster NC, Shah VN. Cannabis Use Is Associated With Increased Risk for Diabetic Ketoacidosis in Adults With Type 1 Diabetes: Findings From the T1D Exchange Clinic Registry. Diabetes Care. 2020;43(1):247-249. doi:10.2337/dc19-0365
Pancer J, Dasgupta K. Effects of Cannabis Use in Youth and Young Adults With Type 1 Diabetes: The Highs, the Lows, the Don’t Knows. Can J Diabetes. 2020;44(2):121-127. doi:10.1016/j.jcjd.2019.05.001







