
Sign up for a new account.
And get access to
The latest T1D content
Research that matters
Our daily questions
Sign up by entering your info below.
Reset Your Password
Don't worry.
We will email you instructions to reset your
password.
You may assume that for someone living with type 1 diabetes (T1D), keeping life-saving glucagon on hand would be a medical necessity. Yet, for many, it’s not that simple, and it’s why this emergency treatment remains underutilized.
Research shows that just over half of people living with T1D have glucagon readily available, which highlights a clear opportunity to increase its adoption.
So what’s standing in the way? Some common barriers to use include cost, insurance coverage issues, short expiration windows, practicality (such as living alone or having never used it before), and perceived difficulties with administering it.
While more research is needed, addressing these obstacles could help more individuals with T1D have emergency glucagon at the ready. Let’s take a closer look.
When hypoglycemia becomes an emergency
Hypoglycemia (glucose < 70 mg/dL) can occur unexpectedly, even overnight. When glucose levels continue to drop into a severe hypoglycemia range (glucose < 54 mg/dL), a person may have a seizure or need the help of others to recover, including glucagon.
This experience can vary from one person to another.
For those having severe low glucose episodes, fear of hypoglycemia (FOH) can occupy equal amounts of mental space as other serious diabetes-related complications.
How does severe hypoglycemia occur? It can be from simple things. Diabetes math gone wrong (too much insulin on board), technology malfunctions, exercise, and even normal daily activities can all contribute to unexpected severe hypoglycemia.
How does glucagon work?
“Glucagon is a medication that can be given to someone who is having a severe hypoglycemic event. That’s when someone’s blood sugar is so low that they pass out (lose consciousness) — or they cannot take things by mouth,” explained Dr. Daniel DeSalvo, MD, a pediatric endocrinologist at Texas Children’s, in a Q&A with T1D Exchange.
“Glucagon can be prescribed in two forms: as an injection or as a medication that’s inhaled through the nose. Both work by helping to mobilize glycogen (glucose) stores in the liver to raise a person’s blood glucose level,” he said.
What’s more, today’s products are injected subcutaneously — in the same spots you use for insulin. They’re far easier to use than the old-style, unmixed powdered glucagon (in a vial) with sterile water (in a syringe), which challenged even well-trained responders.
Plus, with pre-mixed autoinjectors, glucagon can be administered in a few simple steps or even given nasally. Let’s look at the details.
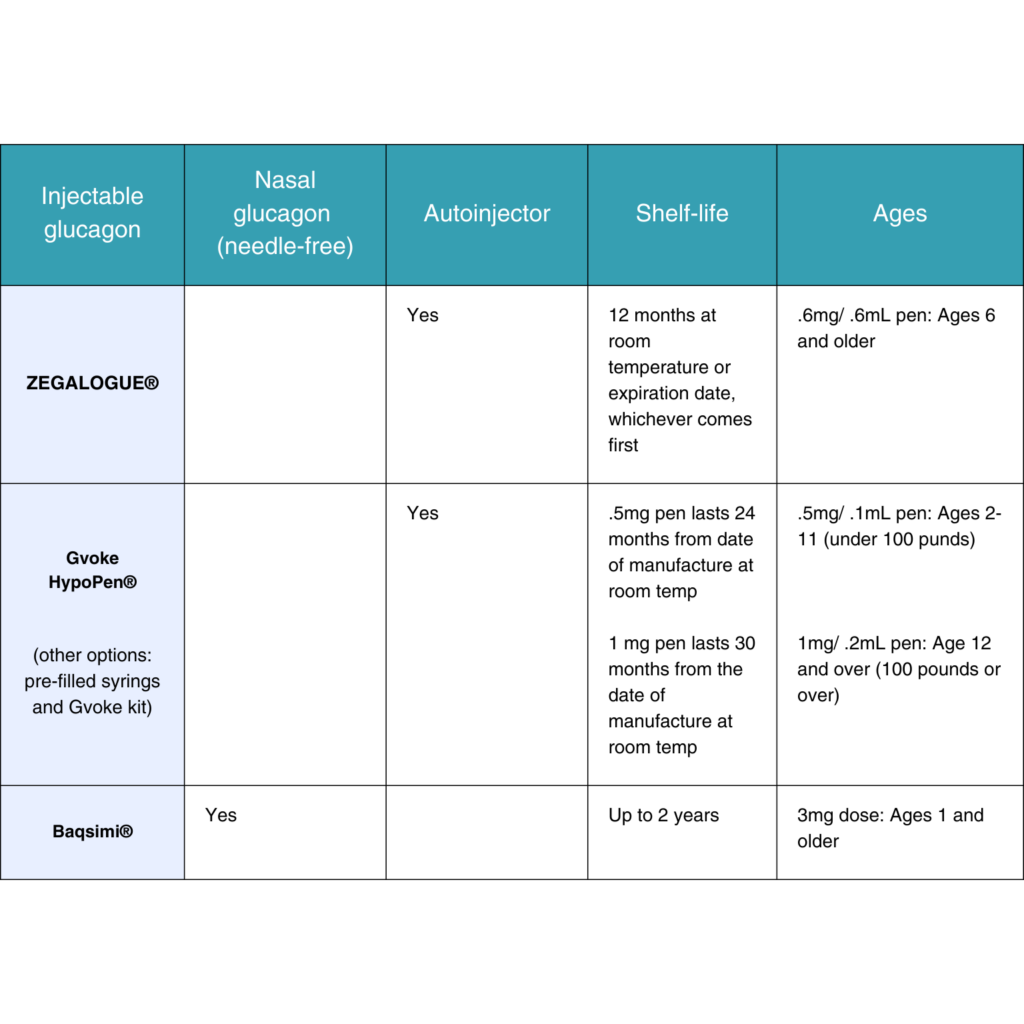
What are the American Diabetes Association (ADA) glucagon recommendations?
The ADA Standards of Care recommend that glucagon be prescribed to all at-risk individuals, including anyone taking insulin or at high risk of hypoglycemia.
Alongside this, individuals living with T1D should receive diabetes education on managing and preventing hypoglycemia, as well as training others in their support network on how to use glucagon in an emergency.
Wanting to learn more from our Online Community, T1D Exchange asked: “Do you have an unexpired emergency glucagon treatment?”
Here’s what they had to say.
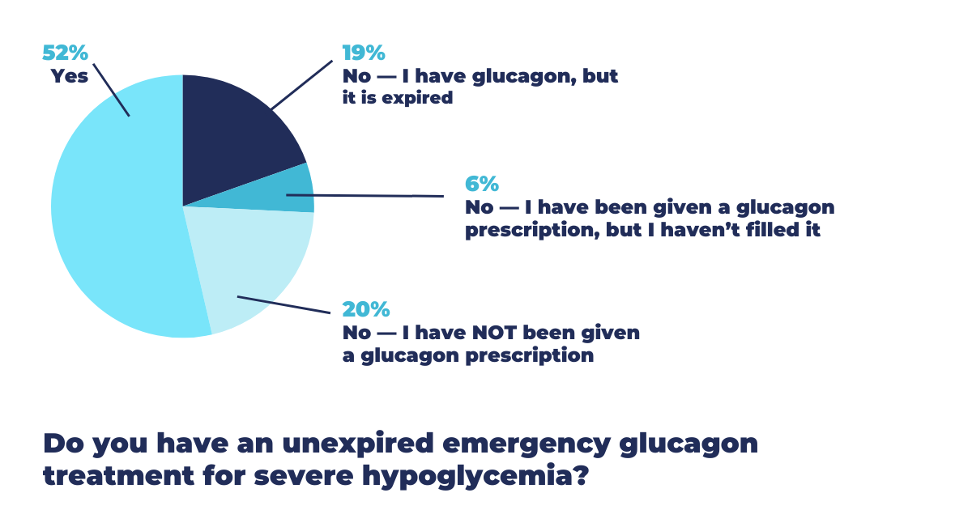
With nearly half of the respondents lacking unexpired emergency glucagon, we sought to understand more about its accessibility. So we asked those who didn’t have it to share why.
Here are some of the responses we received:
- I have expired Baqsimi on hand. I remain confident that it will work, if needed.
- It costs me over $300 to replace it. It’s too expensive.
- Glucagon is $425 for me on Medicare. It’s cheaper to get an ambulance! I have an expired one that will work if I need it, but I won’t.
- Insurance won’t cover, and it was several hundred dollars.
- I’ve never had a glucagon prescription; luckily, I’ve never needed it in 22 years.
- I’ve been a T1D for 57 years. I’ve not had glucagon on hand in 25+ years. Normal carb/sugary items seem to be okay.
- With the latest monitoring technology, I will probably never need it. I needed it a couple of times in the past, many years ago, and I do have expired glucagon on hand. I do question whether expiration ‘is real,’ since until it is mixed, what is there to expire?
- I’ve been taking insulin since 1981. Glucagon has never been mentioned to me by any medical provider, and I have never asked about it.
- No, I haven’t had glucagon in years. The reason is that every time I had a prescription, the glucagon was never used and expired.
- I have that on my list of questions for my endocrinologist — to renew the prescription for my expired glucagon.
What are the most common barriers to having glucagon?
Responses to our question fell into a handful of clear themes. They include:
- Cost: Many said the high out-of-pocket copay (often $300-$400) makes it unaffordable.
- Insurance hurdles: The lack of coverage and the need for prior authorization of the preferred brand can be a hassle.
- Expired stock: Several individuals reported having old, expired kits and were reluctant to replace them.
- “Never needed it”: Some people report never having needed glucagon for a severe low.
- Confidence in other treatment measures: Some people believe that fast-acting carbs, AID systems, and CGMs render glucagon an unnecessary treatment option.
- Limited T1D education: Some providers have never prescribed glucagon, so individuals are unaware of its importance.
- Unfamiliarity: Certain respondents are unaware of new, ready-to-use options that are easier to give.
- Prescription issues: Several never received a prescription, had an expired one, or were prescribed a non-formulary brand.
- Skepticism about expiration: Many respondents believe that glucagon “stays effective after the expiration date,” and don’t feel the need to replace it.
A common mindset was, “I’ve never needed it in the past — why would I need it now?” This mentality can be easy to adopt when expensive kits expire and are often discarded unused.
Here’s what you can do instead: Ask your diabetes care team if they would like your expired glucagon for educational purposes. This can be a win-win, especially for children with diabetes. There are so many people to train, and having hands-on experience with it before an emergency happens helps to build confidence and success.
What if you have insurance but are denied coverage?
If your prescription coverage is denied, stick with it. You have the right to appeal. These steps will help you get life-saving glucagon as a covered pharmacy benefit.
- Talk to your diabetes care team about your situation
- Ask which glucagon is in your insurance plan’s formulary
- Research and ask questions so you understand your rights
- Appeal the decision, include your diagnosis and why glucagon is necessary for your condition
- Have your provider write a letter of medical necessity
Copay cards may help to lower the out-of-pocket cost of glucagon. To get one, visit the manufacturer’s website — such as for the Gvoke HypoPen®, ZEGALOGUE®, or Baqsimi® to see if you qualify.
What if you don’t have insurance?
Without insurance, you’ll want to look into patient assistance programs. These programs can help people get medications for a reduced cost, and sometimes even for free. Again, you’ll want to visit the manufacturer’s website to learn more about the programs they offer.
Wrapping it up
As someone living with T1D and as a parent of a child with T1D, I’ve learned something important: Once you’ve needed glucagon — or given it in a seizure-related emergency for a loved one — you’ll likely have it in your possession forever.







